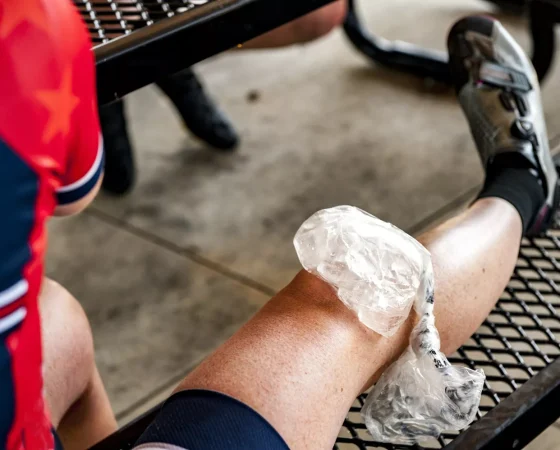
“I’m hurting. Which is better, ice or heat?”
Before we dive into the debate of ice versus heat, let’s first take a look at the healing process. When tissue in our body is damaged from injury or surgery, three phases of healing take place.
Phase 1: Inflammation
Blood vessels dilate and become permeable. Fluid moves from the blood into the interstitial tissue spaces. White blood cells also enter and clean out bacteria and debris, helping to prepare the site for new tissue growth.
Phase 2: Proliferation
New tissue grows and regenerates. Blood vessels nourish new tissue with sufficient oxygen and nutrients.
Phase 3: Remodeling/Maturation
Collagen creates the production of scar tissue, which helps to make the healing tissue stronger.
Cold Indications
I think one of the biggest misconceptions is that inflammation after injury is bad. Cardinal signs of inflammation include pain, redness, swelling, and loss of function. Although these symptoms can be uncomfortable, inflammation is still an important step in the healing process. We recommend cryotherapy (ice, cold packs) during acute inflammation, immediately following injury. It is not to stop inflammation, but to help manage symptoms of swelling and pain by constricting blood vessels (reducing blood flow to the area). We value early controlled movement after injury and since swelling can hinder range of motion, we recommend icing/elevating intermittently 15-20 minutes at a time to reduce negative effects of swelling. Icing can help to numb the area or decrease pain levels, so be sure to set a timer to avoid overdoing it. If you keep the ice pack on for too long, or if it is too cold, the effects become counterintuitive. Your body will notice the lack of blood flow and compensate by sending more blood to the area. We also recommend using a barrier, like a pillowcase or towel to protect the skin from burns/frostbite.
In addition, cryotherapy can help reduce soreness after a physical therapy session or intense workout. Small microtears in the muscle can occur with exercise, but it is the small tears to the muscle that lead to strength and growth. Soreness is normal and a part of muscle building, however icing can be helpful to reduce the intensity of your soreness. Cold temperatures constrict blood vessels, which can also lead to a mechanism that can help flush lactic acid and other wastes out once cryotherapy is removed. Some athletes may participate in ice baths that promote this benefit.
Heat Indications
Heat does the opposite of cold, it promotes blood flow to the area. An increase in blood flow brings oxygen and other healing properties. We recommend heat for tight muscles, restricted soft tissues, stiff joints, or chronic injuries. It can help maximize mobility and can make stretching/range of motion exercises easier. Different types of tissues heal at different rates, depending on the amount of blood flow they receive. For example, muscles heal faster than tendons, because muscle tissue is highly vascularized and gets more blood flow than tendons. This is why tendon injuries can linger much longer and have a higher risk of becoming chronic. The main benefits to heat include improving circulation, increasing soft tissue extensibility, and promoting relaxation. Remember to not apply heat to recent injuries, as that will only exacerbate symptoms of inflammation.
Conflicting Beliefs
Remember, anything that reduces inflammation can also delay healing. This concept has become controversial and bears the question– to ice or not to ice? In 1978, Dr. Gabe Mirkin coined the acronym R.I.C.E., which stands for rest, ice, compression, and elevation after injury. While this method is still commonly practiced, Dr. Mirkin has since recanted this philosophy and no longer advises the components of complete rest and icing. He states that those two methods can actually delay healing. Instead, he recommends early movement after an injury. Research studies are inconsistent and the benefit to icing remains inconclusive. My advice is to keep the injury timeline in mind (ex: was the injury a few days, weeks, months, or years ago?). If ice helps manage your pain and swelling during the acute phase of inflammation immediately after injury, I don’t see anything wrong with that. Anecdotal evidence supports that analgesic effects can be beneficial in reducing reliance on pain medications. In other words, due to its pain relieving effects, some may prefer icing instead of taking pain medication to manage pain.
If the injury was longer than a few weeks or months ago, you are no longer in the acute phase of inflammation. You may wonder, why am I still swollen? Swelling, also known as edema, comes from an increase in lymph fluid to an affected area. Lymph is a clear to white fluid made of white blood cells (lymphocytes). Our lymphatic system regulates movement of lymph to filter out waste, manage fluid levels within our body, and protect us from infection. Just as our blood flows through blood vessels, lymph fluid flows through lymphatic vessels. During a traumatic injury or surgery, these lymphatic vessels can get damaged, thus leading to prolonged swelling.
Lymphatic Circulation
Another way to manage swelling (without cryotherapy or constricting blood flow) is to improve lymphatic circulation. Movement of the body and the affected body part can help this process (ex: pumping the ankle and moving it in different directions after spraining it). Elevating the injured body part above heart level is another strategy to maximize the benefit of gravity. This ushers fluid out and back into the vessels, so it can ultimately be excreted out. Wearing compression garments is another way to reduce excess swelling. At Complete Physical Therapy we utilize vasopneumatic devices. These devices can be worn like a sleeve or pants, and create compression by gently squeezing the affected body part and promoting lymph movement. Lastly, we also perform manual techniques (also known as manual lymphatic drainage massage) to stimulate lymph movement. This light touch massage helps to clear fluid in the tissues and move it out towards lymph nodes.
Conclusion
Do we want to increase blood flow or do we want to decrease blood flow to the area? The answer to this question will help provide insight on whether cold or heat is best indicated. What feels best? Trial and error can also help you assess whether either is a benefit. It is important to note that every case is individualized and each person may respond to injury with varying levels of swelling. Icing and heating modalities can manage symptoms, and we value a combination of relative rest and early controlled movement after an injury to maximize function and optimize recovery!
Photo credits:
https://www.verywellhealth.com/ice-or-heat-2548807