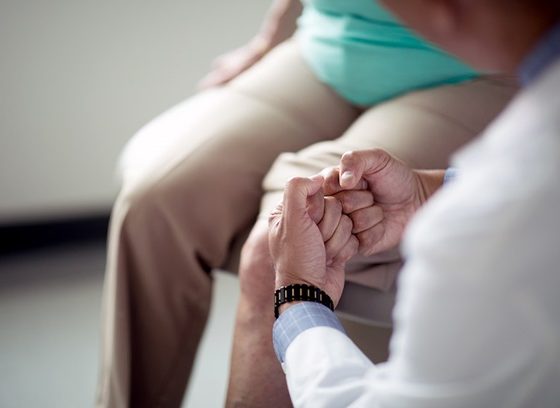
What to Expect After Surgery
Expect to have bruising throughout the thigh and down the leg (even into your foot). This is completely normal, as you have just gone through an extensive surgery. Depending on your surgeon, you may have staples or adhesives securing the incision. To help avoid DVT/blood clots, and to manage swelling, you may be instructed to wear a TED hose or compression stocking. Invest in a good ice pack and wedge to elevate prior to surgery. Icing and elevating your knee intermittently throughout the day/night will be helpful for swelling and pain management. Some surgeons may prescribe pain medications or encourage over the counter pain relievers. Talk with your doctor to determine what options are best for you.
Plan to start PT as soon as possible after your surgery. Be sure to schedule your appointments a couple of weeks ahead of time to ensure appointment times that work best for you and/or family members taking you to PT. We typically see patients within two days post-op. Although you will be feeling sore and swollen, it is important to move the knee. The main goals within the first few weeks include: 1) managing pain/swelling, 2) improving mobility (bending and straightening the knee), and 3) strengthening your quad muscles. You may ask your doctor or physical therapist about “pre-hab” to start exercises beforehand to prepare you for the upcoming surgery. This head start can be very beneficial and help make the rehab process easier.
Prioritize Range of Motion Exercise
Think about all of the activities of life that require bending and straightening of the knee. Our job is to help you reach a “functional” range of motion value, which is approximately 125 degrees flexion (bending) and 0 degrees extension (straightening). Reaching full mobility is important for functional activities of life such as walking, using the stairs, squatting, getting out of the car, stepping over barriers/objects, tying your shoes, riding a bike, and getting up and down from the floor. In addition to bending the knee, it is vital to regain full knee extension (straightening) to maximize quad muscle activation. This muscle engages during knee extension and supports your body weight when walking (it helps prevent you from buckling or falling).
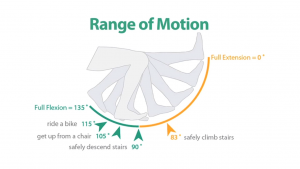
It is essential to regain this motion back within the first 4-6 weeks. As your body heals, scar tissue will develop in the joint, making the knee stiff and inflexible. There is a time sensitive window of opportunity to restore motion, and early stretching is crucial in reducing the risk of immobility. If this is not prioritized, scar tissue adhesions can leave you with a limp and ongoing pain.
Pain
In addition to prioritizing mobility, pain management is important early on in the rehab process. Staying on top of your pain medications and/or other pain relieving strategies, such as icing/elevating and moving the knee throughout the day, will help you stay on track with your progress. One of the biggest challenges with this rehab is the level of discomfort some may experience with range of motion (ROM) exercise. Although it will be uncomfortable, do not let pain deter you from performing your ROM exercises outside of therapy. Also understand that you will not damage the integrity of the replacement by stretching into discomfort. Your physical therapist will help encourage and guide you. They will also be helpful in providing manual (hands on) therapy to release tight muscles, work out scar tissue, and mobilize the joint.
Pain can also be detrimental to sleep quality; which can adversely affect your healing, energy levels, and mood. We recommend you follow your doctor’s guidance of administering pain medication and icing your knee before going to bed. Trial different sleeping positions such as the recliner or sleep on your back in bed. We encourage elevating the leg on pillows or a wedge so it is resting in a straight position. If you are a side sleeper, you may find it difficult to sleep that way in the first few weeks. If you must, remember to sleep on the non-operative side and put pillows in between your legs.
Strength, Stability, and Balance
Once mobility is restored, it is time to progress strength and stability. It is also time to learn how to use your leg again and become confident bearing weight with activities such walking, climbing stairs, getting out of chairs, etc. Physical therapy will help you build your strength back for other activities and exercises you want to return to doing.
Another valuable component of physical therapy is what we call “neuromuscular re-education.” This is the retraining of your muscles, nerves, and brain to work together to improve awareness of your movement and coordination of your body. As an example, your physical therapist will teach you how to walk with proper mechanics, help you break old habits, and basically retrain your body to move normally again! Reducing these compensatory or faulty movement patterns is vital to maximize your recovery. Additional balance exercises and dynamic activities will prepare you for unlevel ground surfaces, improve your balance strategies, and most importantly, reduce your risk of falling.
Fatigue and Endurance
Oftentimes a person’s endurance and stamina will decrease following surgery. This will steadily improve, however being aware of these changes can
help you from “overdoing it.” If you push your limits, your body will let you know. This can result in increased swelling and pain, which may feel discouraging. For example, tasks such as cooking meals and going grocery shopping may require more seated breaks than normal. It is important to recognize your limits, but remember that too little activity can be just as bad as too much activity. Finding a medium level of activity is the goal. Over time, you can gradually start to increase your activity levels to build your endurance back up.
Knee replacement rehab is a marathon, not a sprint. Based on your swelling, range of motion, and the integration into new activities, some days will be better than others. Remember, it can be an undulating (up and down) process, so don’t feel disheartened if things don’t improve each visit. Keep working hard and trying your best. Time and patience is sometimes the biggest hurdle to overcome. Your strength, confidence, coordination, and endurance will all continue to improve as you progress toward achieving your goals.